Brian Morgan – The structural make-up of bacteria, and the development of antibiotic resistance – Nov 2025
Structure of Bacteria– basic description.
Bacteria are around us everywhere. They are to be found in the soil, air and water, and they live inside and outside the human body, some even being essential to the normal workings of our digestive systems and our general health.
Here are sketches of a few of the many kinds that exist, and also a sketch of the structure of a basic bacterial cell.
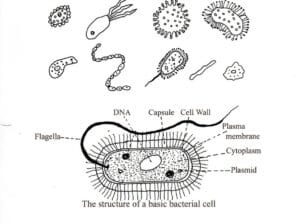
The body of a bacterium is made of protoplasm, a gel-like liquid, which is full of different molecules, water and salts.
The bacterium’s body is surrounded by a thin semi-permeable and elastic membrane that is then surrounded by a rigid cell wall which can be both porous and semi-permeable.
The cell contains proteins, and nucleotide complexes that contain the cell’s DNA and RNA. It is also watery, and this part is known as the cytoplasm.
The cells of bacteria have two basic shapes, spherical and rod-shaped.
The rod-shaped ones also have variants that can be comma-shaped, spiral or filamentous – see sketch below. Some bacteria have additional parts that are fixed to the outside wall of the cell. These can be flagellae for movement, fimbriae for adhesion to surfaces, and other hair-like pili which are similar to fimbriae and are involved in the external transfer of genetic material, including the development of antibiotic resistance. These structures on the surface of bacteria are the ones mostly involved in transferring infections.
In most cases, when a bacterium reproduces the cell usually divides across its middle after putting in place a separating membrane, along with a doubling of its contents before separation. This reproduction can be extremely quick at times, with a new cell being formed within fifteen minutes.
The cell’s DNA, which carries genetic and hereditary material, is held inside the nucleotide.
RNA is ribonucleic acid, which carries the genetic material from DNA to the ribosomes, which direct the synthesis of proteins.
Nuclear Bodies are to be found within the cell nucleus, and they organise genetic activity through the basic building blocks of nucleic acids, like RNA and DNA.
The genetics of bacteria are complicated, and I will try to keep my descriptions of these to a minimum. Videos describing these matters are readily available online.
Bacteria by shape : there are two basic types. Spherical, like a ball; and Rod-shaped which can also be comma-shaped, spiral or filamentous.
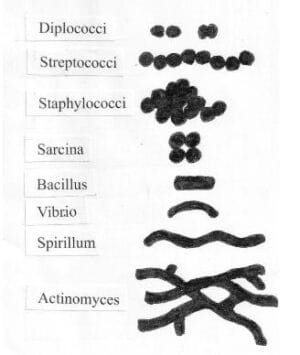
This sketch shows these in the following order:
Diplococci : they are spherical shape and arranged in pairs (diplococcus = “double cocci”).
Streptococci : they tend to form pairs or chains which may appear bent or twisted.
Staphylococci : they appear spherical (cocci) and form in grape-like clusters.
Sarcina : they are spherical and form as packages or bundles.
Bacillus and Vibrio : Bacillus are found on land, and Vibrio in the sea. Both are rod-shaped with vibrio cells curved.
Spirillum : they are long and spiral in shape.
Spirochaete and Actinomyces : Both are rod-shaped. Spiropaetes is spiral in shape, and Actinomyces are filamentous.
Basic bacterial cell shapes
Broad Classification of Bacteria
Hans Christian Gram in 1884 found he was able to classify bacteria according to the thickness of their outer cell wall. He did this by comparing the degree of staining when a dye, crystal violet, is applied to them. Those bacteria that retained its violet or purple stain he called ‘Gram Positive’, and those bacteria which did not he called ‘Gram Negative’.
The Gram Negative group, which do not retain the stain, contains the following bacteria which are all dangerous due to their high antimicrobial resistance to antibiotics:
Pseudomonas, Klebsiella, Proteus, Salmonella, Providincia, Escherichia, Morganella, Aeromonas, and Citrobacter.
The Gram Positive group, which do retain colour on staining, contain the following:
Staphylococci, Streptococci, Pneumonococci, Bacillus anthracis, and Corynebacterium diphtheriae.
Bacteria are also categorised by their shape, as the diagram has shown.
Bacteria are very small, about a fiftieth of a human hair. That is to say, their size is from about 0.2micrometres to 2.0 micrometres (a micrometer is one-millionth of a metre).
Another difference between Gram Positive and Gram Negative bacteria is that, whilst both will have a cell membrane that houses the cell’s cytoplasm (see diagram), known as the cytoplasmic membrane, Gram Negative bacteria will also have an additional membrane that houses the cell outside of its cell wall, whereas Gram Positive bacteria do not have this additional outer membrane.
The cytoplasm within the inner membrane of both types of bacteria will also contain a number of specialized sub-units, known as ‘organelles’. Each organelle has a specific function, similar to organs in the human body that perform different functions. They are responsible for essential cellular activities like energy production, protein synthesis, and storing genetic information. Examples of organelles are mitochondria (energy), the nucleus (genetic information), and ribosomes (protein assembly).
Bacteria also have a surprising number of subgroups, and they can be placed into different categories.
How dangerous can bacteria be to us? -Virulence Factors.
The essential factor of virulence is so often overlooked.
Pathogenspathogens A virus, bacterium or parasite which causes disease is a pathogen. Disease causing pathogens live in the environment, and both humans and animals are hosts to them. Pathogenic viruses, bacteria and parasites are present in sewage, originating from humans and animals, and thus it is essential that sewage is given proper treatment in order to disable (kill) these pathogens before the end-products of sewage treatment (solids and water effluent) are returned to the environment.: Bacterial pathogens are classified in two broad groups: opportunists, and primary pathogens.
Opportunists rarely cause us disease but occasionally can do, especially if we already have health issues.
Primary pathogens are able to cause disease in healthy individuals with good immune reactions. Some of these infections are highly fatal.
But how are the dangers posed to us by bacteria measured? This complex concept is called virulence.
Virulence: There are factors which govern this, called virulence factors. Virulence factors are molecules, structures and mechanisms that allow the bacterium to cause disease in a host. They by-pass the patient’s immune system, and then colonise and damage cells.
Toxins: The various subtypes of bacteria can produce toxins (poisons) of two types. They are:
Exotoxins: they are highly toxic, secreted proteins produced by bacteria that can cause disease by damaging host cells or interfering with cellular functions
Endotoxins: they are complex molecules that cause a potent immune response, potentially leading to fever, organ failure and septic shock.
Enzymes: Bacteria use enzymes of two types. An enzyme is a protein that acts as a biological catalyst, speeding up specific chemical reactions without being used up in the process. The two types used by bacteria are:
Proteases: these enzymes break down antibodies and the outer structures of host cells.
Collagenase: these enzymes break down collagen, the protein that holds cell tissue together. They dissolve the connective tissues and DNA, thus easing invasion of the cell by bacteria.
Surface factors: These are the external appendages of bacteria, like their pili and flagella which enable adhesion (the ability to stick to something). Also, surface factors are the properties of bacteria such as their electrical charge, hydrophobicity (the ability to repel water), and roughness.
Surface factors are of three types:
Adhesins: these are the factors that allows the bacteria to attach themselves to a cell, such as using their pili, and to then colonise the cell through adhesion.
Capsules: these are sticky substances (capsules) that bacteria apply to the protective layers of a cell’s surface in order to stop immune cells from surrounding the bacteria.
Biofilms: these are a protective outer layers which encase colonies of bacteria, preventing attack from outside by immune cells and antibiotics.
Secretion Systems: These are the systems that bacteria use to transport and inject proteins and toxic substances into the cells they are invading, thus making invasion easier. There are four different types, and they generally work together. They work by:
Cellular damage, where toxins disrupt and damage the host cell.
Evading the immune system, where sticky surface substances (capsules) protect the invading bacteria from attack by the immune system.
Attachment and colonisation, where pili and similar features enable the bacteria to stick to the cell that they are invading, and where biofilms are made by bacteria to surround them with an external protective layer to shield them from attack and damage.
Invasion and spread, where collagenase enzymes are used to break down the tissues of the cell being invaded, so making the invasion easier.
Resisting bacterial invasion: The presence or absence of any of the above systems are indicators of degrees of virulence, and it is essential to understand these processes in developing strategies for treating bacterial infections.
Mechanisms of Antimicrobial Resistance
Antimicrobial resistance develops when bacteria evolve different mechanisms to evade the actions of antibiotics. Some bacteria may be able to neutralise an antibiotic to make it ineffective. Others might be able to pump the antibiotic out of their system, or change their own outer wall so the antibiotic cannot attach to it. Bacteria can also alter their own genetic content by mutation in order to resist the antibiotic.
Note: In modern medicine, an antibiotic (also known as an antimicrobial) is a drug that is used to treat infections caused by bacteria and other microorganisms.
The methods of antimicrobial resistance are broadly categorised below:
Intrinsic Resistance
They can change parts of their structure. This is dependent on whether they have a cell wall or not.
Acquired Resistance
They can develop resistance to an antibiotic to which they were previously susceptible. Some can develop a new genetic mutation themselves. Others can import resistant DNA from a nearby resistant bacterium.
Genetic Change
The bacteria’s DNA can change and alter their normal production of protein, so that it does no longer respond to that particular antibiotic.
DNA Transfer;
Bacteria can share genetic material from resistant bacteria through horizontal genegene A string of the DNA (deoxyribonucleic acid) molecule that is the fundamental unit of inheritance, so it is variations in the make up of this molecule in the gene that controls variations in an organism's appearance and behaviour. Genes are found in the nucleus of the organism's cells. transfer. There are three different processes for this. They are:
• conjugation, involving direct cell-to-cell contact via a pilus to enable the transfer of genetic material.
• transduction, using viruses, known as bacteriophages, as carriers.
• tranasformation, where a bacterium takes-up free-floating DNA from its environment.
More specifically, as they come under attack by antibiotics, bacteria are developing their own methods of self-protection. This showed up in the early days of modern medicine with antibiotic resistance in some of the sulphonamide antibiotics. Since then, and for over three decades, antibiotic resistance has been reducing the effectiveness of penicillin.
There are five principle methods of antibacterial resistance adopted by bacteria:
Degradation by enzymes: This involves direct attack on the antibiotic by enzymes produced by the bacterium to denature the antibiotic.
Modifying the target of the antibiotic: This alters the target structure in the bacterium so that the antibiotic cannot bind to it.
Reducing the uptake: This reduces the porosity of the outer membrane so that the antibiotic cannot pass through it.
Efflux pumping: Inside the bacterium there are protein transporters in the cell membrane, and these actively pump the antibiotic out of the cell.
Forming Biofilms: Bacteria can encase themselves in a glutinous protective layer, and this protective layer (biofilm) makes entry by antibiotics into the colony more difficult.
It is essential to understand that these mechanisms of defence arise from the ability of bacteria to develop or acquire resistance genesgene A string of the DNA (deoxyribonucleic acid) molecule that is the fundamental unit of inheritance, so it is variations in the make up of this molecule in the gene that controls variations in an organism's appearance and behaviour. Genes are found in the nucleus of the organism's cells. often from neighbouring bacteria and to adopt them into their own construction.
By natural evolutionary adaptation, bacterial pathogens have developed genetic adaptability by a range of complex means. The development of antibiotics revolutionised medicine, fortunately around the time of World War II, and have become essential to meet the growing challenges of modern medicine, but their effectiveness is now constantly facing new issues.
One of these issues is the inevitable self-protective response of pathogenic bacteria to develop resistance. So far, this has introduced new and dangerous hazards into modern medicine through a lack of preventive treatments. This threat is one of the most serious facing humans in the modern world, and is already leading to greatly increased fatalities due to antibiotic resistant pathogens.
Another of the issues is biofilms. They are a real problem in hospital transmission of infectious diseases, and some are very resistant to standard disinfectants, especially when inside plumbing.
From an evolutionary viewpoint, bacteria have two main strategies:
1. The mutation of genes within the bacterium.
2. The transfer of genes and DNA coding. This happens by horizontal gene transfer between bacteria within the same protective biofilm.
Once the new and resistant mutant has developed, the pathogenic bacteria with the new antibiotic resistance become dominant, and take the lead.
Resistance to one class of antibiotic can be by more than one pathway. Each bacterium can use one or more of the pathways in the development of its antibiotic resistance, and some bacteria seem to prefer a particular combinations of these pathways.
The most successful of these has been producing enzymes, which either destroy the antibiotic or prevent it reaching its target.
There are also regional differences where mutations have developed in isolation, and this can give rise to genetic changes with a highly complex development of subtypes and varieties. In some cases, the protective outer membrane of the bacterium is reinforced, and the access pores made smaller.
Finally, there are mechanisms by which the offending antibiotic is pumped out of the cell, known as efflux pumping. As a result, more infections are becoming difficult to treat and some almost impossible.
Therefore, different tactics like new and greatly improved techniques for hygiene are needed to lessen transfer especially in hospital settings.
References:
Reygaert, 2018: An overview of the antimicrobial resistance mechanisms of bacteria. AIMS Microbiol.
Savin et al, 2021: Antibiotic-resistant bacteria, antibiotic resistance genes, and antibiotic residues in wastewater from a poultry slaughterhouse after conventional and advanced treatments. Scientific Reports 11.
Casadevall, 2009: Virulence factors and their mechanisms of action: the view from a damage-response framework. Albert Einstein College of Medicine.
Peterson, 1997: Bacterial Pathogenesis. Medical Microbiology 4th edition. https://www.ncbi.nlm.nih.gov/books/NBK8526/
Venkateswaran et al, 2023: Revisiting ESKAPE Pathogens:virulence, resistance, and combating strategies focusing on quorum sensing. https://pubmed.ncbi.nlm.nih.gov/37457962/
Woolhouse et al, 2015: Antimicrobial resistance in humans, livestock and the wider environment. The Royal Society, B, Philosophical Transactions.
Fluit et al, 2001: Molecular Detection of Antimicrobial Resistance. Clinical Microbiology Reviews, American Society for Microbiology.
Storms et al, 2020: The Virulence Index: A Metric for Quantitative Analysis of Phage Virulence. https://www.liebertpub.com/doi/10.1089/phage.2019.0001#
Peterson 1996: Bacterial Pathogenesis – Medical Microbiology.


























